Structure Of The S Protein
With a size of 180200kDa, the S protein consists of an extracellular N-terminus, a transmembrane domain anchored in the viral membrane, and a short intracellular C-terminal segment . S normally exists in a metastable, prefusion conformation once the virus interacts with the host cell, extensive structural rearrangement of the S protein occurs, allowing the virus to fuse with the host cell membrane. The spikes are coated with polysaccharide molecules to camouflage them, evading surveillance of the host immune system during entry .
The total length of SARS-CoV-2 S is 1273 aa and consists of a signal peptide located at the N-terminus, the S1 subunit , and the S2 subunit the last two regions are responsible for receptor binding and membrane fusion, respectively. In the S1 subunit, there is an N-terminal domain and a receptor-binding domain the fusion peptide , heptapeptide repeat sequence 1 , HR2 , TM domain , and cytoplasm domain comprise the S2 subunit . S protein trimers visually form a characteristic bulbous, crown-like halo surrounding the viral particle . Based on the structure of coronavirus S protein monomers, the S1 and S2 subunits form the bulbous head and stalk region . The structure of the SARS-CoV-2 trimeric S protein has been determined by cryo-electron microscopy at the atomic level, revealing different conformations of the S RBD domain in opened and closed states and its corresponding functions .
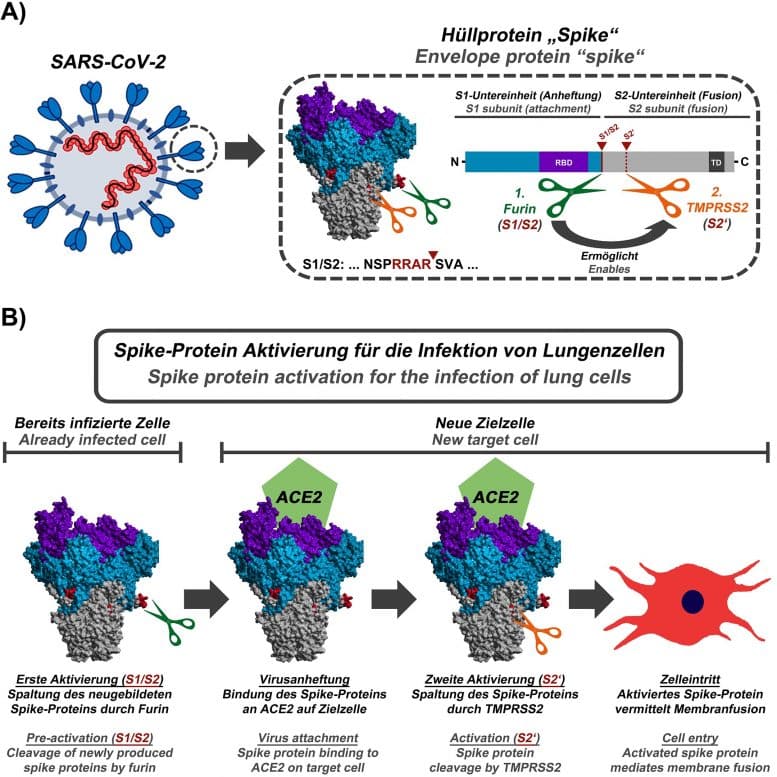
Fig. 2: Structure of the SARS-CoV-2 S protein.
What Do Antibodies Do
Antibodies are another kind of protein. They take a Y-like shape, and their job is to recognize such intruders as bacteria and viruses in your body.
How do they do that? The tips of the Y are slightly different from antibody to antibody. Your body makes billions of different antibodies, which mostly differ at the tips. The tips shape, the molecular composition and charge has to be exactly right to fit on the end of the spike protein and block it. Once the tip of the spike protein is blocked, then it cannot fit into the ACE-2 receptor anymore. So this is what is called a neutralizing antibody.
The other thing antibodies can do is, once theyre attached to the spike protein, they can act like a flag. And then other immune cells can recognize that flag and say OK, I gotta go eat this thing. This is a thing thats bad for the body.
Once our body has the instructions to make the spike protein, it is able to do a really good job of building up antibodies to block the spike proteins.
Types Of Vaccines: Mrna Viral Vector And Protein Subunit
Currently, there are three main types of COVID-19 vaccines that are approved or authorized for use in the United States: mRNA, viral vector, and protein subunit. Each type of vaccine prompts our bodies to recognize and help protect us from the virus that causes COVID-19.
None of these vaccines can give you COVID-19.
- Vaccines do not use any live virus.
- Vaccines cannot cause infection with the virus that causes COVID-19 or other viruses.
They do not affect or interact with our DNA.
- These vaccines do not enter the nucleus of the cell where our DNA is located, so it cannot change or influence our genes.
Don’t Miss: Should I Use Protein Powder
Coronavirus Spike Protein Activated Natural Immune Response Damaged Heart Muscle Cells
Research Highlights:
- Researchers have demonstrated for the first time a potential route of the SARS-CoV-2 spike protein damaging the heart.
- In study evaluating mice and human heart cells, the SARS-CoV-2 spike protein inflamed the heart muscle cells, which can lead to heart injury.
Embargoed until 8 a.m. CT/9 a.m. ET, Monday, July 25, 2022
CHICAGO, July 25, 2022 Heart damage is common among patients hospitalized with COVID-19, leading many to wonder how the virus affects the heart. Now, researchers have found that the spike protein from the severe acute respiratory syndrome coronavirus 2 virus can lead to heart muscle injury through the inflammatory process, according to preliminary research to be presented at the American Heart Associations Basic Cardiovascular Sciences Scientific Sessions 2022. The meeting, held in Chicago on July 25-28, offers the latest research on basic and translational cardiovascular science.
The spike protein is found on the surface of SARS-CoV-2, the virus that causes COVID-19. Spike proteins latch onto receptors known as angiotensin-converting enzyme 2 on target cells. The spike protein facilitates virus entry into healthy cells, which is the first step in infection. In addition to infecting the lungs, the virus can also spread to other organs leading to more damage to the body, severe infection and, among some people, death.
Additional Resources:
About the American Heart Association
For Media Inquiries and AHA Expert Perspective:
How Long Do Mrna And Spike Proteins Last In The Body
Vaccines generally work by introducing a piece of a virus or bacteria into your body so you can develop long-lasting immunity to the pathogen. While the piece introduced by the vaccine rapidly fades away, your body’s immune system remembers what it saw. When it encounters the virus or bacteria in the real world it mounts a strong immune response preventing or decreasing the severity of infection.
Some have expressed concern that the spike protein or other parts of the mRNA vaccines build up in the body, particularly in the ovaries or the brain. Here we break down the data to show where mRNA vaccines travel in the body. There is no evidence that any mRNA or protein accumulates in any organ.
You May Like: High Protein Diet Constipation Relief
Functions Of The S Protein
The S protein on the surface of the virus is a key factor involved in infection. It is a trimeric class I TM glycoprotein responsible for viral entry, and it is present in all kinds of HCoVs, as well as in other viruses such as HIV , influenza virus , paramyxovirus , and Ebola . Similar to other coronaviruses, the S protein of SARS-CoV-2 mediates receptor recognition, cell attachment, and fusion during viral infection .
The trimer of the S protein located on the surface of the viral envelope is the basic unit by which the S protein binds to the receptor . The S1 domain contains the RBD, which is mainly responsible for binding of the virus to the receptor, while the S2 domain mainly contains the HR domain, including HR1 and HR2, which is closely related to virus fusion .
Protease Inhibitors Targeting Sars
SARS-CoV-2 entry requires cleavage of the S protein at the S1/S2 and S2 sites. Proteolysis by TMPRSS2 and cathepsin B and L plays an important role in priming SARS-CoV-2 S for entry. Camostat mesilate is a potent serine protease inhibitor of TMPRSS2. Utilizing research on the SARS-CoV and SARS-CoV-2 cell entry mechanism, it has been demonstrated that SARS-CoV-2 cellular entry can be blocked by camostat mesilate . There are currently five clinical trials registered to evaluate the efficacy of camostat mesilate . In addition, cathepsins in lysosomes are crucial for SARS-CoV entry via endocytosis. E-64d, an inhibitor of cathepsin L, blocks infection with SARS-CoV and SARS-CoV-2 PsV . Future trials with COVID-19 patients may help to confirm the efficacy of E-64d therapy.
Phosphatidylinositol 3-phosphate 5-kinase is the main enzyme synthesizing PIP2 in early endosomes . Apilimod, a potent inhibitor of PIKfyve35, can significantly reduce the entry of SARS-CoV S pseudovirus into 293/hACE2 cells via early endosomes in a dose-dependent manner . Treating 293/hACE2 cells with another PIKfyve inhibitor, YM201636 , also had a similar effect. Moreover, a major downstream effector of PIP2, two-pore channel subtype 2 , is important for SARS-CoV-2 entry, and tetrandrine inhibits the activity of SARS-CoV-2 S pseudovirus.
Read Also: Fiber One Chewy Protein Bars
How To Protect Your Ace2 Receptors And Detox Il
Spike protein attaches to your cells ACE2 receptors, impairing the receptors normal functioning. This blockage may alter tissue functioning and could be responsible for triggering autoimmune disease or causing abnormal bleeding or clotting, including vaccine-induced thrombotic thrombocytopenia.
Ivermectin, hydroxychloroquine , quercetin and fisetin are examples of substances that may naturally protect your ACE2 receptors. Ivermectin works in this regard by binding to ACE2 receptors, preventing the spike protein from doing so.
Interleukin 6 is a proinflammatory cytokine that is expressed post-injection and levels increase in those with COVID-19. Its for this reason that the World Health Organization recommends IL-6 inhibitors for people who are severely ill with COVID-19. Many natural IL-6 inhibitors, or anti-inflammatories, exist and may be useful for those seeking to detox from COVID-19 or COVID-19 injections:
- Boswellia serrata
Ways The Spike Protein Harms The Body
During the two-plus years of the COVID-19 pandemic, many studies have analyzed the effects of the spike protein from different aspects, and have discovered that it is harmful to the human body in several ways, including:
1. Damaging the lung cells 2. Damaging the mitochondria and DNA structures 3. Damaging cardiovascular cells 4. Increasing the risk of blood clots 5. Damaging brain cells 8. Increasing the risk of cancer
We will go into the details of each of these points.
Recommended Reading: Best Protein Powders For Weight Loss
How Long Mrna Lasts In The Body
The Pfizer and Moderna vaccines work by introducing mRNA into your muscle cells. The cells make copies of the spike protein and the mRNA is quickly degraded . The cell breaks the mRNA up into small harmless pieces. mRNA is very fragile that’s one reason why mRNA vaccines must be so carefully preserved at very low temperatures.
Preventing Spikes Shape Change
To initiate an infection, the spike proteins must bind to the ACE2 receptor. They then dramatically change shape, folding in on themselves. This enables the virus to fuse its membrane with our own cells membranes and get inside. However, as Chen and colleagues reported in 2020, the spikes in the original SARS-CoV-2 sometimes prematurely changed shape and fell apart before the virus could bind to cells. While this slowed the virus down, the shape change also made it harder for our immune system to contain it.
Because the original spike protein would dissociate, it was not good enough to induce a strong neutralizing antibody response, says Chen.
But when Chen and colleagues imaged the mutant spike protein, they found that the D614G mutation stabilizes the spike by blocking the premature shape change. Interestingly, the mutated spikes bind more weakly to the ACE receptor, but the fact that theyre less apt to fall apart prematurely renders the virus more infectious overall.
Cryo-EM structures of the original and mutated SARS-CoV-2 spike protein
Say the original virus has 100 spikes, Chen explains. Because of the shape instability, you may have just 50 percent of them functional. In the G614 variants, you may have 90 percent that are functional. So even though they dont bind as well, the chances are greater that you will have infection.
You May Like: High Protein Low Sugar Bars
What Are Mrna Vaccines And How Do They Work
Vaccines help prevent infection by preparing the body to fight foreign invaders . All vaccines introduce into the body a harmless piece of a particular bacteria or virus, triggering an immune response. Most vaccines contain a weakened or dead bacteria or virus. However, scientists have developed a new type of vaccine that uses a molecule called messenger RNA rather than part of an actual bacteria or virus. Messenger RNA is a type of RNA that is necessary for protein production. Once cells finish making a protein, they quickly break down the mRNA. mRNA from vaccines does not enter the nucleus and does not alter DNA.
Like all vaccines in the United States, mRNA vaccines require authorization or approval from the Food and Drug Administration before they can be used. Currently vaccines for COVID-19, the disease caused by the SARS-CoV-2 coronavirus, are the only authorized or approved mRNA vaccines. These vaccines use mRNA that directs cells to produce copies of a protein on the outside of the coronavirus known as the spike protein. Researchers are studying how mRNA might be used to develop vaccines for additional diseases.
Glycan Shield Of The Sars

As mentioned earlier, the SARS-CoV-2 S proteins are heavily decorated by heterogeneous N-linked glycans projecting from the S trimer surface. The SARS-CoV-2 S sequence encodes up to 22 N-linked glycan sequons per protomer, which likely plays an important role in protein folding and host immune evasion as a glycan shield . Of the 22 potential N-linked glycosylation sites on the S protein, 14 were identified to be predominantly occupied by processed, complex-type glycans . The remaining eight sites were found to be dominated by oligomannose-type glycans, which are divergent from those founded on host glycoproteins . Although glycosylation sites proximal to the receptor-binding sites on the SARS-CoV-2 S protein can be observed, ACE2 bound to the glycosylated and deglycosylated S ectodomains with nearly identical affinity determined by a biolayer interferometry binding assay . This observation suggests that the high binding affinity between the SARS-CoV-2 S protein and ACE2 does not depend on the S protein glycosylation.
Recommended Reading: Foods High In Protein Vegetarian
What Is The Ace2 Receptor
The ACE2 receptor is located in the cell wall, in lung and blood vessel linings, and in platelets. Spike protein attaches to ACE2 receptors.
It has been proposed that large concentrations of spike protein may bind to our ACE2 receptors and effectively sit there, blocking the regular functioning of these receptors in various tissues. The disruption of these receptors has been associated with a multitude of adverse effects through altered tissue functioning.
- If spike proteins bind to the cell wall and stay put, they could trigger the immune system to attack healthy cells and possibly trigger autoimmune disease.
- The spike protein could attach to ACE2 receptors located on blood platelets and the endothelial cells lining the blood vessels, which may lead to abnormal bleeding or clotting, both of which are linked to Vaccine-induced Thrombotic Thrombocytopenia
What You Need To Know
- COVID-19 vaccines help our bodies develop immunity to the virus that causes COVID-19 without us having to get the illness.
- Different types of vaccines work in different ways to offer protection.
- None of the COVID-19 vaccines can give you COVID-19.
- Bringing new vaccines to the public involves various steps, all which must be followed before they are made available for use.
Don’t Miss: Protein Shakes For Pregnant Women
Vaccine Vs Spike Protein
Given how crucial the spike protein is to the virus, many antiviral vaccines or drugs are targeted to viral glycoproteins.
For SARS-CoV-2, the vaccines produced by Pfizer/BioNTech and Moderna give instructions to our immune system to make our own version of the spike protein, which happens shortly following immunisation. Production of the spike inside our cells then starts the process of protective antibody and T cell production.
One of the most concerning features of the spike protein of SARS-CoV-2 is how it moves or changes over time during the evolution of the virus. Encoded within the viral genome, the protein can mutate and changes its biochemical properties as the virus evolves.
Most mutations will not be beneficial and either stop the spike protein from working or have no effect on its function. But some may cause changes that give the new version of the virus a selective advantage by making it more transmissible or infectious.
One way this could occur is through a mutation on a part of the spike protein that prevents protective antibodies from binding to it. Another way would be to make the spikes stickier for our cells.
This is why new mutations that alter how the spike functions are of particular concern they may impact how we control the spread of SARS-CoV-2. The new variants found in the UK and elsewhere have mutations across spike and in parts of the protein involved in getting inside your cells.
Scientific Journal Articles For Further Reading
Jain S, Venkataraman A, Wechsler ME, Peppas NA. Messenger RNA-based vaccines: Past, present, and future directions in the context of the COVID-19 pandemic. Adv Drug Deliv Rev. 2021 Oct 9 179:114000. doi: 10.1016/j.addr.2021.114000. Epub ahead of print. PMID: 34637846 PMCID: PMC8502079.
Verbeke R, Lentacker I, De Smedt SC, Dewitte H. The dawn of mRNA vaccines: The COVID-19 case. J Control Release. 2021 May 10 333:511-520. doi: 10.1016/j.jconrel.2021.03.043. Epub 2021 Mar 30. PMID: 33798667 PMCID: PMC8008785.
Microscopic image of SARS-CoV-2, the virus that causes COVID-19. Spike proteins are seen surrounding the outer membrane of each virus particle.
Also Check: What Does Proteins Do For The Body
How Long Do Spike Proteins Last In The Body
The Infectious Disease Society of America estimates that the spike proteins that were generated by COVID-19 vaccines last up to a few weeks, like other proteins made by the body. The immune system quickly identifies, attacks and destroys the spike proteins because it recognizes them as not part of you. This “learning the enemy” process is how the immune system figures out how to defeat the real coronavirus. It remembers what it saw and when you are exposed to coronavirus in the future it can rapidly mount an effective immune response.
The Novavax vaccine introduces the actual protein into your body to produce an immune response similar to many other vaccines currently in use.
Do Vaccine Spike Proteins Stay In The Body
As we know, the COVID-19 vaccines have incorporated an expression mechanism for the viral spike proteins that triggers our immune systems to respond to the virus. But the question remains: How long do the spike proteins from the vaccines remain in the body?
The spike proteins are divided into two parts: S1 and S2, with S1 remaining in the blood and S2 bound to the cell membranes.
A study published in Clinical Infectious Diseases discovered that the S1 proteins would appear in humans soon after the first dose of the Moderna vaccine, and that some people would still have intact spike proteins two weeks after the first dose of the vaccine.
The finding that intact spike proteins were still present in people two weeks after vaccination was beyond expectations.
Another study published in the Journal of Immunology found that S2 proteins could still be detected four months after the second dose of the Pfizer vaccine.
However, the harm of spike proteins is related to their amount. The aforementioned side effects are all based on in vitro studies and animal models, and the relatively serious damage occurred only when the amount of spike proteins was large.
If the viral mRNA in the vaccine only appears in small amounts in the muscles and doesnt enter the blood or organs in large amounts, then these serious side effects wont occur. That means clearing out these spike proteins can limit their potential negative effects on the body.
Don’t Miss: Good Sources Of Plant-based Proteins Include